
Most care providers already monitor what matters.
- Falls.
- Pressure damage.
- Weight loss.
- Medication errors.
- Hospital admissions.
- Safeguarding concerns.
These areas are measured, governed, audited and reviewed because organisations understand something important:
Consistency protects residents.
But for many years, foot health sat outside that same level of visibility.
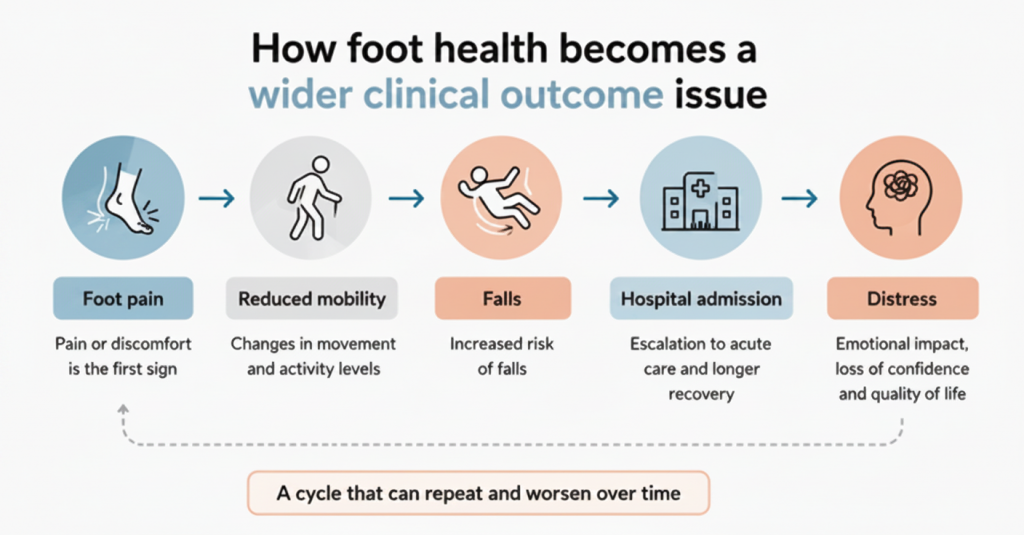
And yet poor foot health impacts almost every one of those wider outcomes.
- Mobility.
- Falls risk.
- Pain.
- Skin integrity.
- Behavioural distress.
- Independence.
- Quality of life.
The challenge was never that providers didn’t care.
Most genuinely do.
The challenge was that foot health evolved historically as a service category without the same governance structures applied to other clinical risks within social care.
And over time, that created significant variation across the sector.
The Invisible Variation Problem
From the outside, many services can appear similar:
- residents are being seen
- visits are taking place
- foot care is “covered”
But underneath that, the level of:
- clinical assessment
- risk identification
- escalation
- documentation
- oversight
- governance
- continuity
can vary significantly between providers.
Often even between homes within the same group.
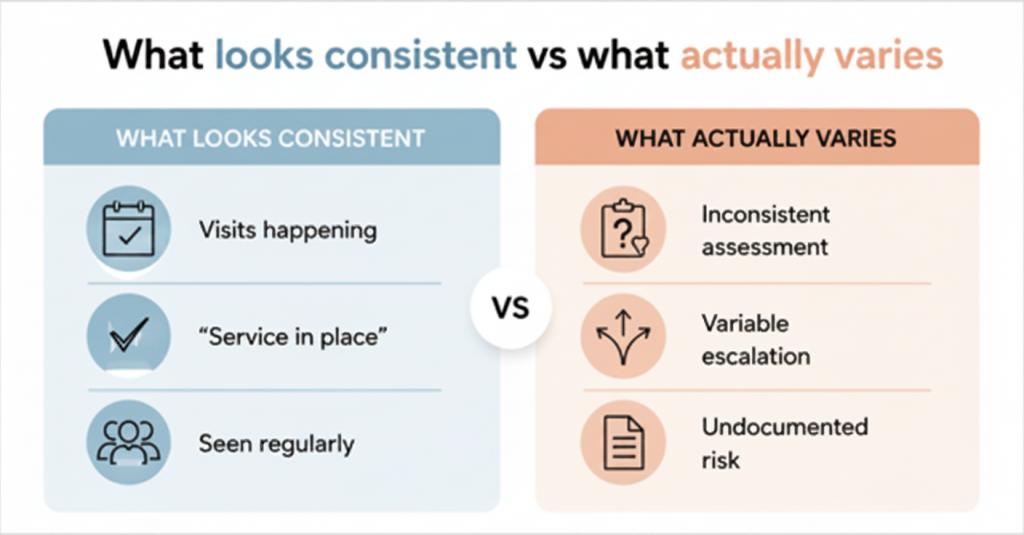
The difficulty is that this variation often remains invisible until it starts showing up elsewhere operationally:
- increased falls
- avoidable pain
- mobility deterioration
- distressed behaviours
- reduced participation
- avoidable hospital admissions
- residents declining care
And by the time those issues become visible, the underlying risks may have been developing for months.
Why Foot Health Was Historically Overlooked
Part of the issue is historical perception.
For many years, foot health within care homes was often viewed primarily as a maintenance or cosmetic service rather than a clinical one.
In some settings, it became grouped alongside non-clinical service provision:
- nail cutting
- comfort care
- appearance-based maintenance
Rather than being recognised as an area connected to:
- falls prevention
- pain management
- tissue viability
- diabetes risk
- infection prevention
- mobility preservation
- behavioural wellbeing
- overall resident health outcomes
As a result, the governance structures surrounding foot health often failed to evolve at the same pace as other regulated areas of care.
At the same time, a significant proportion of foot care provision within care homes has historically been delivered by individuals who are not HCPC regulated clinicians.
Many work incredibly hard and care deeply about residents.
However, differing levels of training, regulation and scope of practice across the sector can create substantial variation in:
- assessment capability
- escalation pathways
- clinical decision-making
- documentation
- safeguarding awareness
- accountability
And currently, there remains very limited national guidance specifically focused on creating consistent governance and assurance standards around foot health provision within care homes.
That creates risk not only for residents, but also for care teams and providers attempting to navigate an area without clear operational frameworks.
The Conversations That Led to the Framework
Over time, our work increasingly moved beyond simply delivering podiatry services.
Providers were asking larger questions:
- How do we know standards are consistent?
- What does good foot health governance actually look like?
- How do we identify risk earlier?
- How do we evidence oversight?
- How do we align foot health with wider organisational quality metrics?
Those conversations eventually contributed to ongoing work alongside Care England around best practice, governance and the development of a white paper exploring foot health within social care.
And one thing became increasingly clear:
Foot health could no longer sit as a reactive standalone service.
It needed to become part of a wider clinical governance conversation.
That is how the Foot Health Assurance Framework™ was developed.
Not as a generic podiatry package.
But as a structured governance model designed specifically for the realities and risks of care home environments.
The Five Pillars of the Foot Health Assurance Framework™
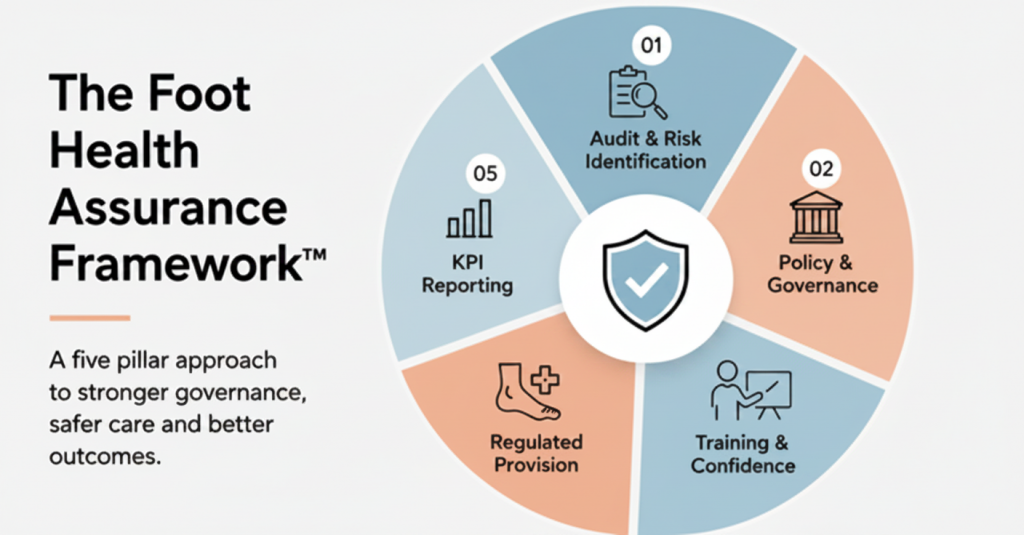
1. Audit & Risk Identification
The first step is visibility.
Many organisations cannot improve what they cannot clearly see.
The framework begins with structured auditing to identify:
- variation between homes
- gaps in oversight
- escalation concerns
- documentation inconsistencies
- resident risk patterns
- operational vulnerabilities
This creates a clearer organisational picture of foot health risk rather than isolated snapshots.
2. Policy & Governance
Many providers have foot care activity in place.
Far fewer have robust governance structures surrounding it.
The framework supports clearer:
- policies
- escalation pathways
- accountability structures
- clinical oversight standards
- documentation expectations
- risk management processes
Helping foot health move into the same governance conversations as other regulated areas of care.
3. Staff Training & Confidence
Care staff are often the first people to notice subtle deterioration.
But historically, many teams have received limited education around:
- recognising risk
- identifying deterioration
- escalation thresholds
- when presentation changes require action
The framework supports targeted education designed specifically for care home environments so teams feel more confident identifying concerns earlier.
4. Regulated Podiatry Provision
Not all foot health provision operates at the same clinical standard.
The framework supports safer and more accountable provision through:
- clearer communication
- stronger escalation
- continuity of care
- defined clinical oversight
- improved documentation
- regulated pathways
Importantly, the focus is not simply on delivering treatment.
It is on ensuring governance exists around the treatment itself.
5. KPI Reporting & Organisational Alignment
One of the most important elements is measurement.
The framework allows foot health to become visible within wider organisational quality conversations.
Including alignment with metrics such as:
- falls
- mobility
- pressure care
- safeguarding
- behavioural distress
- hospital admissions
- resident wellbeing indicators
Importantly, KPI reporting is personalised to each organisation’s existing operational priorities and governance structures.
Because every care group measures success differently.
Why This Matters Now
The social care sector is moving toward greater accountability, visibility and evidence-based governance across all aspects of care.
Foot health cannot remain outside that conversation.
Especially when the downstream impact affects so many wider resident outcomes.
Residents experience the consequences of inconsistency even when systems around them appear stable on the surface.
And increasingly, providers want:
- stronger governance
- clearer oversight
- measurable assurance
- proactive risk management
- consistency across services
- safer escalation pathways
The Foot Health Assurance Framework™ was designed to support exactly that.
A Different Conversation Around Foot Health
This is not about creating unnecessary complexity.
And it is not about criticising providers already working under significant operational pressure.
It is about helping organisations bring greater structure, visibility and consistency to an area of care that has historically operated without the governance frameworks applied elsewhere.
Because when foot health improves, many wider resident outcomes improve alongside it.
Explore the Foot Health Assurance Framework™
Most providers already suspect there is variation in foot health provision across the sector.
What many don’t yet have is:
- a clear governance structure
- meaningful oversight
- measurable standards
- visibility of hidden risks across services
That is exactly why the Foot Health Assurance Framework™ was created.
To help care groups move foot health from a reactive, task-based service into a clinically governed area of resident care with clearer oversight, accountability and consistency.
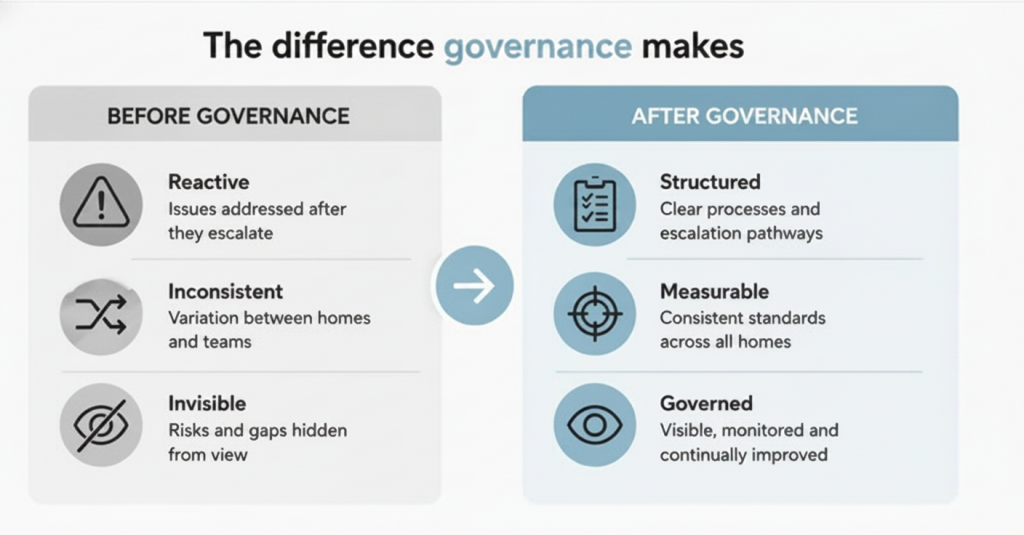
The framework supports providers to:
- identify hidden risks earlier
- improve consistency across homes
- strengthen escalation pathways
- align foot health with wider quality metrics
- create safer and more accountable provision
- increase visibility at governance level
If you would like to explore:
- the 5-pillar framework
- example KPI reporting
- audit structure examples
- governance model in more detail
book a quick Teams conversation



